Monthly Archives: March 2017
Surrogacy in Kenya for Gay Parents
Kenya is one of the most popular and cost effective options for LGBT, heterosexual, married and single parents. Legislation in neither promoting, nor banning surrogacy, meaning that it is not regulated by the law. However, a number of professional clinics and agencies are offering effective treatments and gay parents are wholeheartedly welcome. If you are considering Kenya as a surrogacy destination, you can inform yourself about legislation, service and other details here.
Lately there has been a discussion about how much gay friendly Kenyan society actually is. A lot of sources reinforce the idea that same-sex couples, in general, are strictly discriminated and prejudiced in Kenya. They also suggest to keep sexual orientation discrete not only from the society, but from the fertility clinics as well. The advice is mostly based upon the fact that a lot of religious leaders are quite skeptical about same-sex relationships, not to tell anything about their parenthood rights.
Hiding sexual orientation, not being honest with health care provider on such an important journey is definitely not something gay parents will choose. Why is Kenya such a popular destination then? Why are gay parents having successful results? Why do patients have positive experiences with their clinics? – Just because the spread information and belief is misleading.
Reality
Nairobi , the capital city of Kenya, is developed and modern – even closer to European cities than some cities in Southeast Asia. Travelling there is safe and a pleasant experience. Parents can even combine their visit with unforgettable safari holidays. Tourism is an important sector for Kenya’s economy . Society and doctors too, are usually very welcoming towards tourists, including LGBT couples. It would not be professional if doctors discriminated their patients based on their private lives. What about branches of international and professional surrogacy agencies? Would they send patients to clinics where they will not get treated or will be prejudiced? It simply can not be in their interest.
All around the globe, we encounter members of the society that are accepting, fighting or feeling neutral about every single subject. Attitude towards gay parents, like everything else, is disputable too. Stopping random people, asking for their opinion and inspecting the actual reality are two different things. One should make reasonable assumptions based on experiences and outcomes of others. A good surrogacy agency will not refuse to clarify the issue parents are concerned about – may it be past experiences, statistics or concretely the attitude towards gay parents.
Surrogacy Destinations where Gay Parents are most Welcome
Surrogacy legislation is the matter of constant change. For intended parents, there are a lot of attractive destinations. However, when it comes to choosing one, the process doesn’t seem as simple anymore. Unfortunately, surrogacy destinations are more limited for LGBT parents. We would like to present places, where gay parents are most welcome to complete their journey to parenthood.
The United States
Surrogacy in the United States varies from state to state. In one country, there are places where surrogacy either is banned, not regulated or accepted. Additionally in some states surrogacy is accepted for heterosexual or/and married couples only. However, luckily, there are states where gay parents are wholeheartedly welcome too. Currently, the most surrogacy, as well as same-sex friendly state is sunny California.
Unfortunately, surrogacy costs in the USA may fall in between the price range of 100 000 – 200 000 USD. For that reason, it is not an affordable option for many parents.
Mexico
Similar to the United States, Mexico consists of several states and each has it’s own legislation. A number agencies in Mexico are leading surrogacy programs successfully and are happy to treat patients independent from their sexual orientation. Mostly, they are operating in Cancun and Mexico City. Surrogacy there, is not regulated by the law and is neither legal, nor illegal.
Cancun is definitely a dreamy destination for vacation and for investors accordingly. Due to the increasing number of clinics and foreign investments, compared to the past 3 years the success rate of In Vitro Clinics has grown significantly. Surrogacy prices in Mexico are significantly lower than in the USA.
Asia
Gay parents have been friendly welcomed in southeast asian countries. Not a long ago, surrogacy was banned in most popular destinations – Cambodia and Thailand. However, southeast Asia is not losing the status of cost effective and same-sex friendly surrogacy destination. Lately, Laos has emerged as a popular surrogacy destination and is likely to substitute Cambodia and Thailand. A lot of professional doctors have already moved to Laos from neighbouring countries and continue their successful fertility treatments there.
IVF Success Rates
Nowadays, intended parents have an access to a number of information. This is logical, because future parents in need of an in vitro fertilization (IVF) treatment, have to be familiar with every single aspect of this process. The primary subject to interest is of course the probability of a successful outcome – healthy pregnancy. Surrogacy agencies and clinics tend to make claims about their high IVF success rates. While success rates are an important indicator of clinic’s performance, numbers do not always depict the reality.
Meaning and Calculation
IVF success rates represent the ratio between pregnancies and IVF procedures. One could think of it as – “how many IVF procedures resulted in a pregnancy?”. Many clinics and agencies offer two types of rates to their future patients – clinical pregnancy and live birth success rates.
Clinical pregnancy rates will tell how many IVF procedures resulted in a clinical pregnancy.
Clinical pregnancy rate = number of total pregnancies / total number of IVF procedures.
Unfortunately, pregnancy is not yet a guarantee of a healthy gestation and delivery of a baby. For that reason, the rate intended parents are more interested in, is the one of live births.
Live birth rate represents how many IVF procedures resulted not only in a clinical pregnancy, but also in a delivery. Just because pregnancy lasts about 9 months, clinics and agencies may not have such regularly updated live birth success rates.
Live birth rate = number of total live births / total number of IVF procedures.
What do IVF success rates really tell us?
The higher the success rate of a clinic is, more attractive it seems to patients. However, each patient is much more than a part of a chart. Intended parents have very different problems and needs, they belong to different age groups and come from various medical backgrounds. All of the factors play an important role in the field of fertility. Majority of pregnancies are successful after only several IVF procedures. Even an average young and fertile couple has only a 20% chance of conceiving naturally within a month.
Having a 80% IVF success rate could hypothetically be true, however not for all patients, but rather for certain age groups.
Success Factors
To underline how individual IVF results are, parents should consider factors that play a significant role in successful outcome.
- Age
Age of the mother is one of the main factors in successful IVF. The quality and the amount of eggs become lower when females are over 35. For that reason, it is obvious that women below a certain age are going to have a higher IVF success rate. When intended mother is older than 35, it may be advised to use eggs from a younger donor.
- Pregnancy history
IVF success factors depend on previous pregnancy(ies) of an intended mother. For example, if female has experienced recurrent implantation failure, miscarriages or stillbirths, she will probably have a lower IVF success rate.
- Various fertility problems
Fertility issues are caused by various medical conditions an disbalances. Endometriosis, polycystic ovary syndrome, high levels of FSH and LH hormones just to name few. Accordingly, IVF success rate depends on stages and progression of various health issues.
- Lifestyle
Female smokers tend to need more IVF attempts than non-smokers. Maintaining a healthy body mass index is also a crucial factor in fertility. Over and underweight females, as well as smokers have a lower IVF success rate than ones who lead healthy lifestyles.
Experience, training, dedication and professionalism of the IVF staff is also of a huge importance. IVF success rate is in fact connected with clinic’s general performance and proficiency. However it is not a direct indicator of individual parent’s probability of success.
The keypoint is not to accuse the clinic claiming to have an incredibly high success rate in data manipulation and misinterpretation. Neither is the point to ignore the 80% IVF success rate of a clinic and go for the one that has humbly published the number below 30%. Intended parents only have to know that high IVF success rate of a clinic ONLY is not yet an objective guarantee of desired outcomes and should not play the major role in formation of future plans.
The best way to relate personal situation with IVF success rates data, is to make assumptions based on doctor’s consultation. Based on medical testing procedures, the healthcare provider will be able to make reasonable assumption whether patient is falling in the list of “average” ones.
Surrogacy in the USA
Surrogacy legislation in the United States varies from state to state and is a subject to regular change. While searching for surrogacy options across the country, it is likely to encounter states where it is permitted, banned or not mentioned at all.
There is also a variation between states that do not prohibit surrogacy in terms of accepting commercial surrogacy, unmarried couples, naming intended parents in documents and etc. To save time and narrow down the list of options significantly , we have chosen surrogacy friendly destinations based on best experiences and following criterias :
- Surrogacy is permitted (for heterosexual couples, same-sex couples and single parents)
- Parents are named on birth certificate and have legal assurances
Surrogacy friendly states
- California
- Connecticut
- Delaware
- Maine
- Oregon
- Rhode Island
If intended parents come across a successfully operating surrogacy agency in any other state, it may be still worth a try. Going through surrogacy legislation by state, it is common to find regions where court is generally very favorable despite of not having a corresponding law.
States that intended parents should NOT consider due to the explicit ban currently include : New York, New Jersey, Indiana and Michigan.
It is not simple to talk about surrogacy in the USA due to constant alterations. When reaching out to the surrogacy agency , commissioning parents should clarify all kinds of information about:
- Current surrogacy legislation in the state, recent and possible future changes
- Post and pre-birth orders, who will be mentioned in the birth certificate?
- Requirements for parents (heterosexual, married or in committed relationship, single, same sex and etc)
California, for example, meets expectations for intended parents independant from marital status and sexual orientation – everything accompanied by a guarantee of parenthood rights based on legal documents.
Pricing
Taking into account the scales and level of development we are talking about, it is not a problem to find a well equipped clinic in the United States. However, intended parents should know in advance that the average cost for gestational surrogacy in the USA is between $100-140 000. This is not an affordable option for many parents. Fortunately, there is a number of cost effective options for heterosexual and LGBT parents worldwide.
Embryo Quality and Grading
Can we estimate results of In Vitro Fertilization? What are the chances of a successful embryo transfer? What do embryo quality and grading mean? Do they tell anything about possible outcomes? These are the questions intended parents worry about the most. While embryo grading is a complex medical process, parents need and should be informed about every important step on their fertility journey.
What do Embryo Quality and Grading Mean?
Embryologists use embryo grading system in order to make predictions about embryo transfer results. These predictions do not depict the reality accurately. A lot of embryos with low or middle grading lead to successful pregnancies. Moreover, not all high quality graded embryos result in gestation. This happens mainly because grading does not give an information about embryo’s genetics.
Embryo grading system is still a powerful tool that gives a good impression about which embryos are appropriate for transferring / freezing. Estimating embryo’s quality and potential is an important step. It helps intended parents to save time, finances, protects from unexpected misfortune and may facilitate their parenthood journey.
There is no universal grading system. In some clinics grade 1 is better than 4, while in others 4 may indicate the best quality. The most common practice is to observe an embryo after 3 or 5 days of fertilization. However, embryos are not on the same development stage on these days. Embryologists use different grading systems for day 3 and day 5.
Grading on day 3
On the day 3, embryos are on their “cleavage stage”. This means that cells in the embryo (blastomeres) are dividing. Observation happens under a high power microscope. On the day 3 after retrieval, embryo itself is not growing in size – only the cells are being replicated.
Accordingly, grading criteria number one is the number of cells in the embryo. The desired number of cells on the day 3 is 6-10. Based on experience, embryos containing 6 to 10 blastomeres on day 3, are more likely to result in successful pregnancy.
Criteria number 2 is the presence of fragmentation. Fragmentation/Blebbing is the process when the inside of the cells break off and form fragments. These blebs do not contain nucleus. Nucleus is the cell storing cell’s genetic material, DNA. As fragments/blebs are separated from the nucleated part of the cell, they are not referred to as cells. It is preferable to have little or no fragmentation at all. On the other hand, embryologists may capture multinucleation (presence of more than one nucleus per cell). Multinucleation is very hard to identify but may unfortunately indicate chromosomal abnormality of the embryo.
Embryo quality and grading includes one more important criteria – cell regularity. It is desired that blastomeres are of the same or close to the same size.
After the observation on the day 3, embryos having no fragmentations and including equally sized 6-10 cells will be considered of high quality and will be assigned the highest grade. Laboratory will assign further grades according to their own system. The higher the quality grades are, so is the likelihood of successful implantation.
Grading on day 5
On the 5th day after fertilization,embryo contains increased number of cells and a fluid cavity. As the cells are growing, they start to form in different types. We encounter two cell types on the day 5. First type forms the Inner Cell Mass (ICM) and the second one is called Trophectoderm Epithelium (TE). Day 5 embryo is referred to as Blastocyst and has reached the development stage when it is getting ready to attach itself to the uterine lining (Implantation).
ICM will grow into fetus and TE will form pregnancy essential tissues. Due to their importance for gestation, day 5 grading system evaluates both cell types separately. ICM and TE will be both observed for their amount and density (how tightly are they packed). For example a lot of tightly packed cells indicate higher quality than loosely packed fewer ones.
Blastocyst should implant soon. Above mentioned cell types divide and fluid cavity has to enlarge and hatch out of its shell. Fluid cavity’s volume in the embryo is one more criteria of 5th day grading. It should begin to outgrow the space inside of the shell (zona pellucida) and then the blastocyst will be ready for the implantation.
Day 5 embryo will be assigned the higher quality grade, when fluid cavity has reached the appropriate volume, ICM is tightly packed, is sufficient in amount and TE is also forming a cohesive layer with sufficient quantity of cells.
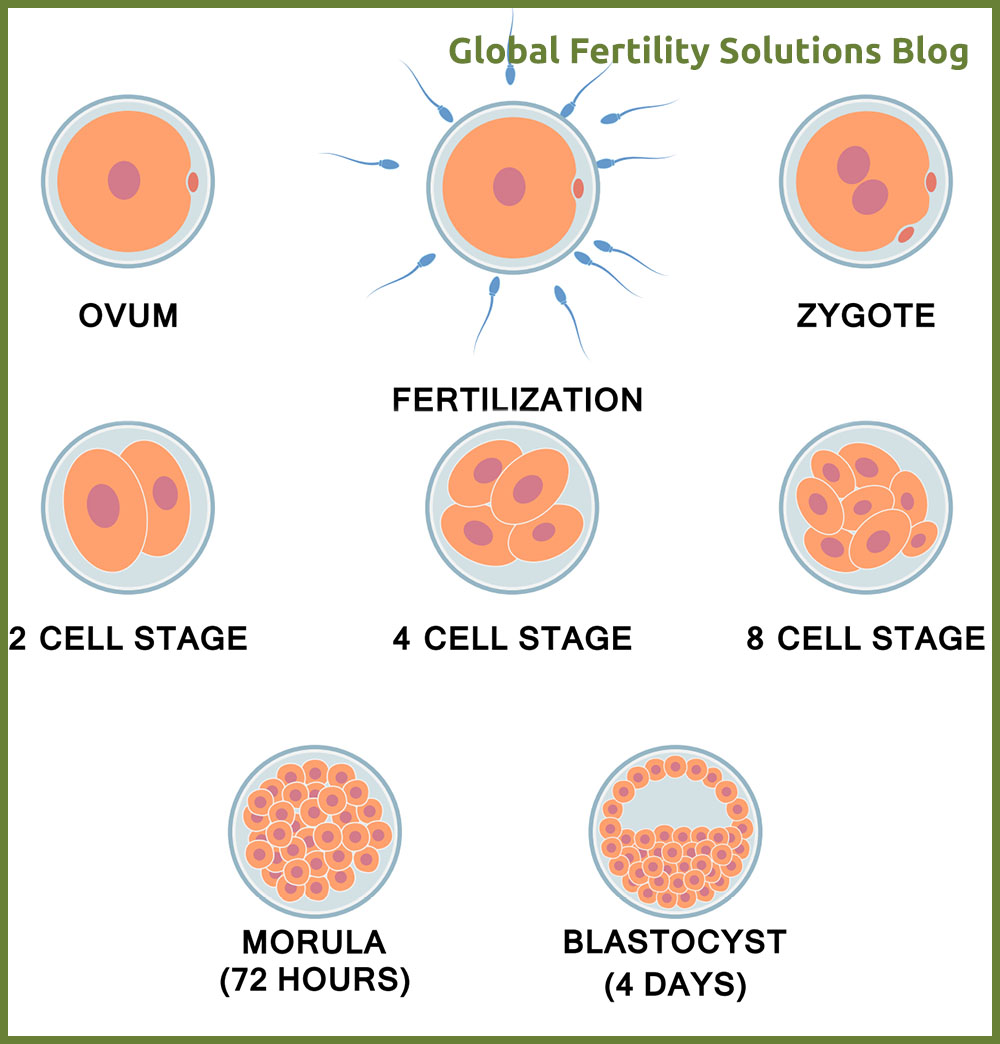
As already mentioned, clinics may use different grading systems and utilize numbers or symbols to assign grades. However, most of the laboratories use exactly above mentioned criterias to evaluate the potential of an embryo.
While talking about the chances of successful gestation, high embryo quality and grading is not a 100% guarantee. There are far more details included in the successful outcome. Sometimes an embryo does not implant because it has a genetic or chromosomal abnormality. It also happens that a lower grade embryo results in an unproblematic gestation because it has healthy genetics. A lot of clinics will suggest doing preimplantation genetic screening(PGS). This procedure checks chromosomal normality in the embryo.
Positive results in PGS and middle to high graded embryo already give a reasonable purpose to estimate a healthy pregnancy.
Surrogacy – Possible Medical Risks
Gestational surrogacy is an emotionally overwhelming process. Finding a professional surrogacy agency, preparing for the program, going through IVF, transferring an embryo to surrogate and waiting for the positive results… There are more details in between these steps.
It is a great relief when everything is completed successfully and your gestational carrier(surrogate mother) is now bearing your baby. The most complicated and complex tasks are already left behind. The fact that embryo transfer and implantation was successful is already a huge step forward.
Gestational problems are not very likely to occur to a surrogate mother and we will further explain why. However, because there is still a chance that pregnancy can go wrong, intended parents should be informed about possible medical risks of surrogacy.
Health of a surrogate mother is observed and monitored intensively before admitting her to the program. Her medical history must be absolutely suitable for a future pregnancy. A lot of agencies require that surrogate is already a mother to a healthy child. Unhealthy habits (smoking, drinking alcohol and etc) have to be absent absolutely. Intended parents are and should be allowed to request any information concerning their gestational carrier’s medical and mental health. After such a close observation and control, surrogate mother is very likely to have a successful pregnancy and deliver a healthy child.
However, let us address possible medical risks of surrogacy anyway.
Possible medical risks
Surrogate mothers, similar to any other females are likely to experience slight weaknesses that accompany nearly every gestation. Symptoms may include :
- Sickness
- Mood swings
- Change in appetite
- Nausea
- Slight abdominal and lower back pain
If any of the symptoms are no longer mild and cause a serious discomfort, surrogate mother should address a healthcare provider and inform the surrogacy agency as soon as possible.
Severeness of any symptom may lead to miscarriage, preterm labour and other serious complications. Pregnancy may seem healthy but it is still possible for gestational carriers to experience common types of pregnancy complications (gestational diabetes,preeclampsia and so on). Baby might inherit genetic abnormality from intended parents that needs to be captured on time.
As already mentioned, surrogate mothers may experience mood swings. Sometimes it is emotionally intimidating to carry a baby for 9 months, monitor your and his/her health throughout the process, go through labour and finally have to give the baby up (independent of having no biological connection to the child).
If needed, surrogate mothers should have the ability to attend therapies. Agency should explain to them the distribution of roles in surrogacy and reinforce the position of both sides in legal documents.
What should be done for the best results?
First of all, commissioning parents have to discuss all scenarios with their surrogacy agencies :
- What are the medical risks of surrogacy?
- What will happen if gestational mother has pregnancy complications?
- How do we know that surrogate visits doctors regularly?
- What is the backup plan?
- How are we sure that surrogate will give up the child? (This is not an issue in countries where surrogacy is regulated by the law – Ukraine and Georgia are perfect examples.)
Commissioning parents should request and receive regular information about :
- Surrogate mother’s health
- Baby’s health
- The course of pregnancy
- Test results
Surrogacy agency, on the other hand, is responsible for :
- Controlling surrogate’s visits to health care provider
- Collection of medical data
- Informing intended parents
Independent from their motivation , surrogate mothers are doing an amazing job delivering babies to their biological parents.To avoid any kind of complications and medical risks, like any other female – lifestyle, mental and physical health of gestational carrier has to be monitored on regular basis.
Implantation Failure
Journey to parenthood is sometimes full of obstacles and challenges. Before reaching a healthy pregnancy, female organism has to complete several complicated stages. It happens that our bodies are not always capable of dealing with their tasks. Implantation failure is one of the most frustrating experiences on the way to parenthood. We have to learn about ways of helping our bodies to conduct required processes successfully.
What is implantation?
Once an egg is fertilized successfully, female body starts to prepare for pregnancy. Walls of the uterus start to thicken and grow in order to protect and nourish embryo throughout the following 9 months of gestation. Wall of the uterus is called endometrium and is where the fertilized egg attaches itself for further growth and development. The process of attachment is called implantation.
Accordingly, when we refer to implantation failure, we mean that fertilized egg was not able to attach itself to the wall of the uterus.
Implantation is probably one of the most complicated processes before the successful pregnancy. Implantation failure may contribute to unexplained infertility in females. Abnormalities that occur during implantation are indeed complicated to capture.
Assisted reproductive technology (ART) stands for procedures that aim to achieve pregnancy through surrogacy, in vitro fertilization (IVF), egg donation and etc. Throughout ART programs, implantation failure is one of the most common occurrences. While IVF is an amazingly successful treatment of infertility, not all cycles tend to result in successful implantation.
Recurrent implantation failure
Recurrent implantation failure refers to inability to achieve pregnancy after four embryo transfers, provided that embryos are of a good quality. Unfortunately up to 10% of females experience implantation problems during their IVF treatment.
Some of the related tests and factors include :
- White blood cells, leukocytes , are responsible for protecting body from infections and “invaders”. Increased level of white blood cells are found to contribute to recurrent failure of cycles. Doctors, however, may suggest to not treat this issue. It is a controversial and confusing task to treat infertility by suppressing the immune system – which is so important later during the pregnancy. Drugs suitable for treatment can be risky for mother and a child. Before the beginning of treatment, parents should consider discussing all of the possible outcomes with their doctors.
- Endometrial scratch is the procedure when doctor passes a thin catheter through cervix. Disruptions caused by catheter rotation result in response within the endometrium and surprisingly is found to have a positive effect on endometrium ability of reception. Doctor may also pass a thin telescope into the womb and observe if there is a polyp or a scar tissue that needs to be removed.
- It is available to observe a tissue from endometrium to find an underlying problem. Scientists claim that it is possible to analyze a number of genes (more than 200) that are associated with implantation.
- Clotting of the blood is a further factor that can hold pregnancy from progressing. Doctor might prescribe medications to thin the blood as a part of treatment.
While controlling health of parents is essential, experience revealed that the cause of implantation failure is usually hiding behind egg quality and rarely behind sperm or uterus.
- Preimplantation genetic screening is the process of removing a cell from IVF embryo and testing it for genetic conditions and chromosomal abnormalities. Studies suggest that maternal age is the typical reason behind chromosomal abnormality in embryo. If several IVF attempts are unsuccessful, using a young egg donor is likely to result in normal pregnancy. Together with female’s age, abnormalities in mature eggs increase correspondingly.
It is particularly hard to make predictions about implantation. Scientists still have a long way to go until they investigate this stage closely. However, above mentioned tests and facts are proved to be relevant while discovering and solving the issue.
Surrogacy in Russia
Surrogacy in Russia was first practiced in 1995 and has become a popular destination for foreign patients gradually. A lot of surrogacy agencies and clinics are operating successfully and are promising to deliver the best results. However there have been several doubts about choosing Russia as a surrogacy destination. By going through the surrogacy legislation and regulations in Russia, we will discuss all of the important issues to be aware of.
Legislation
Surrogacy is legal and is regulated by the Family Code of Russia. According to the law, commissioning parents are not required to be married and single parents are also allowed to participate in programs. Foreigners are welcome.
Intended parents have to provide a medical assessment that proves their inability to become parents without assistance. This could include :
- Uterus absence or deformation
- Somatic diseases that do not allow / are dangerous for pregnancy
- History of several IVF failures
Surrogate Mother
Surrogate mother is required to have at least one healthy child of her own. Her medical and mental state must be checked and observed carefully before admitting her to the program. Surrogate mother can not be an egg donor at the same time. However, despite the absence of genetic connection with the child, surrogate mothers still have full parental rights for babies. Gestational mother gives parenthood rights to commissioning parents only with her consent.
Commercial surrogacy plays a major role in solving the problem. Fortunately it is legal in Russia to pay a surrogate mother for the service of carrying pregnancy(similar to Ukraine, Georgia and some states of the USA). A lot of gestational mothers see surrogacy as an opportunity to live better lives with their families. Surrogacy agencies and clinics are also promising to handle all of the legal aspects themselves. However, it is still strongly advised to work with the family law agency throughout the surrogacy period.
Service and Costs
Surrogacy programs are offered in several Russian cities. Of course, the most popular destination is the capital city – Moscow. Apart from being a popular tourist destination with picturesque views and great history, Moscow offers a number of medical centers with modern equipment. Surrogacy agencies have years of experience and are indeed reliable companions on the journey to parenthood. Average cost of IVF, medical care and legal support is on average 40-50 000 $. This price is considered to be affordable for surrogacy and is somewhat higher than the average cost in Ukraine, Georgia and Kenya, but still half of the price in the USA.
Surrogacy in Russia has no doubt a lot of advantages to go for – affordable prices, experienced agencies and clinics, well equipped medical centers. However, intended parents should note that there have been several cases when surrogate mothers refused to give up their parenthood rights. We would strongly encourage intended parents to use service of a lawyer throughout the entire process of surrogacy. Lawyer will negotiate with the gestational carrier from the very beginning and prepare all of the documents for abnegation of parenthood rights. If something goes wrong, family lawyer will also represent intended parents in court.
